My mother, who was native Norwegian, didn’t speak much Norwegian at home to me and my 3 siblings. She was more interested in losing her accent and becoming American. We would say our dinner prayer in Norwegian and she would sing a Norwegian lullaby at night as she tucked us into our feather bed, a sleeping luxury imported from Norway not yet commonly found in America in the 1960’s. She would use Norwegian words to describe our anatomy and bathroom habits, a secret language we were able to use in whispered tones while seated in the pew of our church on Sunday morning: “I need to go to the bathroom!” During the holidays my mom’s culture would emerge as we danced and sang around the tree on Christmas Eve. On Easter, we would go cross country skiing wearing knickers and long wool socks and worship the sun.

My two older brothers learned to speak Norwegian on a year abroad in Norway after high school, as did my younger sister, to some degree. After my graduation, instead of going to Norway, Annie, my high school sweetheart and I, welcomed a child into the world and our lives changed forever. We were 18 year old parents blessed by a daughter that has now blessed us with two grandchildren. I knew then and have always known that missing a year abroad and starting a family was my destiny. Two sons followed and we now have 8 grandchildren. If I felt any remorse at all about not going to Norway it was put to rest twenty years later when our daughter spent a semester abroad at the University of Bergen, a short train ride from my mother’s hometown where our relatives still live and my mom is buried.

I wasn’t a very good student in high school. I was often kicked out of chemistry class for not paying attention in class — I prefer the term day dreaming — and although biology was intriguing, my curiosity for living things didn’t translate well to testing. I preferred the storytelling of my history teachers, the humanity of my English teachers, and the awakening I felt in art class, especially the photography dark room where any knowledge of chemistry beyond basic safety wasn’t necessary. I was delighted at how I could frame the world through a camera’s view finder and then watch an image magically appear on silver halide photosensitive paper in the red light of the darkroom as I gently rocked the tray of developer.
I was required to take 2 years of a foreign language in high school in order to graduate. I choose Spanish since many place names in my Northern California community were in Spanish. We lived near the El Camino Real, the Spanish Colonial Mission system that dotted the California coastline with 21 Missions from San Diego to Sonoma. We lived just miles from the San Rafael Mission just north of San Francisco. I was an average student in Señor McSween’s Spanish class, distracted by his bushy eyebrows nested over his blue eyes, a righteous comb over, and his distinctly bad American accent when he spoke Spanish.
When I was diagnosed with cancer in my early 40’s I began instruction in another language — the language of cancer. My education came at me all at once like water rushing from a broken dam overwhelming me as I tried to stay afloat in the confusion and uncertainty of a life threatening disease. As the diagnosis settled in and the realization of the necessary surgery to remove my cancerous bladder was clear, I decided knowledge was my only way forward. I needed to learn as much as I could about my body, the whole of my human anatomy, how the mutated cells inside my bladder were multiplying, what the four stages of cancer really meant, how chemo and radiation would help and hurt me, the function of the cerebellum where my cancer spread, and the cerebrospinal fluid and the neural axis where it also spread.
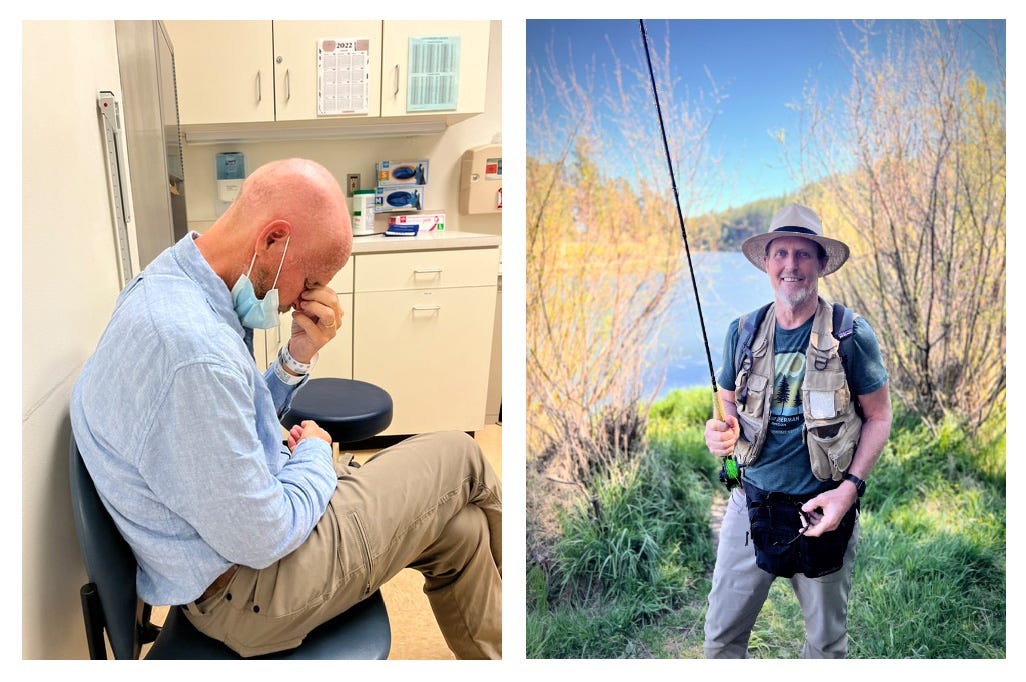
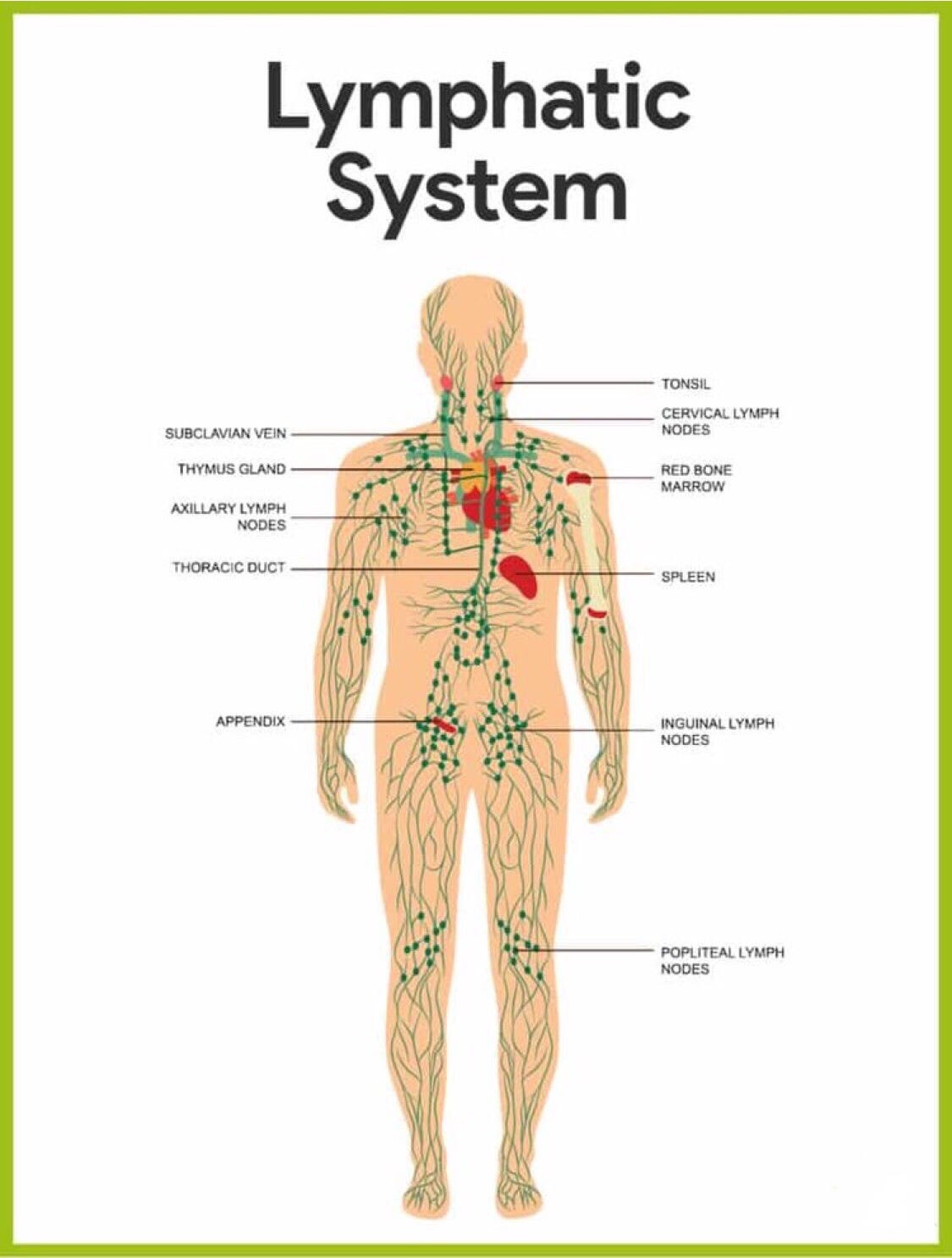
I was particularly interested in the lymphatic system, a network of vessels and tissues carrying clear, watery fluid made in the bone marrow that flows through our bodies collecting and destroying abnormal cells like viruses, bacterial infection and cancer cells. Unlike the heart that pumps blood through our circulatory system, the lymphatic system has no similar pump. It moves though the body by the physical movements we make and through respiration where every breath moves the ribs and chest wall in and out to move the fluid. Microscopic cancer cells can hide out for years, and then erupt in distant lymph nodes, as it did in my body.
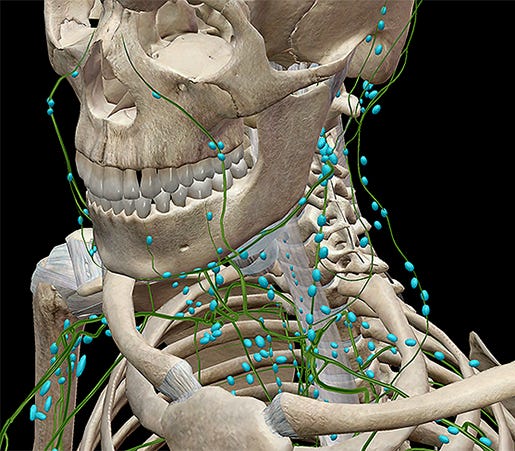
The human body has around 800 lymph nodes. The cancerous cells collected by the lymph fluid and trapped in the lymph nodes is eliminated through aptosis, a form of programmed cell death where white blood cells called phagocytes — monocytes, macrophages, and neutrophils are all phagocytes — ingest the pathogens and damaged cells. The lymph fluid is then recirculated into the blood stream through lymphatic ducts in the chest. When my cancer returned after a 12 year remission it emerged in my lymph nodes: groin (inguinal), rectum, pelvis (iliac), abdomen (paraaortic and mesenteric), chest (hilar and mediastinal), under arm (axillary), under my collar bones (surpraclavicular) and neck (cervical and occipital). The cancer bypassed my visceral organs — typical locations for bladder cancer to spread are the bones, liver and lung — and eventually went straight to my brain and spine.
I became immersed in the culture of cancer where my new-found language skills helped me to decipher the multitude of acronyms used in my CT scans and MRI reports — Computed Tomography and Magnetic Resonance Imaging — and especially in research papers related to clinical trials. Here’s a brief list of a few abbreviations I’ve become familiar with:
PD-1 & PD-L1 — programmed cell death one & programmed cell death ligand one
mAb — mono clonal antibody, as in Pembrolizamab, the immunotherapy I’m currently on
CCR — continuous complete remission
CR — complete remission / complete response
CAR-T — chimeric antigen receptors and T cells
DFI — disease-free interval
DFS — disease-free survival; time without disease prior to relapse
EFS — event-free survival; time from diagnosis to defined events (relapse or death)
NED — no evidence of disease
PD — progressive disease
OS — overall survival
PFS — progression Free Survival
RFS — relapse-free survival; time from diagnosis to relapse or death
PR — partial response, partial remission
TTP — time to progression
SD — stable disease
Lymphocytes known as T-cells and B-cells normally track down and eliminate unwelcome invaders like damaged DNA within cells that can quickly replicate out of control and grow into a tumor. These T and B cells are part of the adaptive immune system (AIS) and can usually identify very specific features of these pathogens. In cancer, the immune system isn’t able to identify the proteins on the cancer cell allowing the cancer to spread throughout the lymphatic system and metastasize to distant parts of the body.
Checkpoint inhibitors (PD-1/PD-L1 )have been developed to help the immune system recognize cancer cells and destroy them. It’s like the immune cells, the T-cell and B-cell, has been given a key to unlock the protein on a cancer cell that has disguised itself from the immune system and can continue to multiply and grow. Once unmasked, the T-cells recognize the bad actors and eliminate the cancer, but, as a side effect, have a tendency to over amplify the immune response and attack healthy tissue, just like an auto-immune disease. Immunotherapy works in roughly 20-25% of patients and only in certain cancers. It’s not a cure but may extend life many months, or even years in some patients. The odds of working are increasing with combination therapies and new therapies like CAR-T (Chimeric Antigen Receptor T-cell therapy) where they remove patient’s T-cells and alter them in the lab and return them to the patient. The results have been remarkable, especially in blood cancers.
I learned the language of cancer, not for a letter grade, but as an act of survival. My curiosity about every procedure, scan report, treatment plan, blood draw results, and charts of survival curves has made me an informed patient able to converse with my doctors about my disease. I can decipher research papers well enough to stay current on new treatments. It has made me a better advocate for bladder cancer.
The same wonder I felt in the darkroom where my love of photography was born and led to a life in the visual arts is the same wonder I have for the way scientists tinker within the DNA of our human cells in the lab in search of a cure. My 20 year cancer survivorship is due, in part, to this marriage of science and art, one discipline informing the other, rocking slowly between each like a tray of developer, an image emerging in the future where the language of cancer is no longer necessary.






I love the way you relate the wonder you feel for the magic of science to the magic of photography. I practice photography too and just posted an essay on the similarities between writing and photography. I had a gynecological cancer in 2022, I'm in remission but there's a pelvic lymph node they are watching. Fascinating read, thank you.
Another expertly crafted essay on life and learning. Thank you for sharing your story with us Lars.